
Now there has been a lot of fussing about just what constitutes an HIE as well as the bigger issue of how do the feds insure that HIEs of one form or another are in place to support the MU criteria for information exchange. Looking at the slides that the HIE Workgroup used for this meeting, it appears that they were attempting to first educate the broader committee on just what an HIE may be, what types of data may flow through an HIE in support of MU criteria and finally some recommendations to consider for HIEs to support overarching HHS objectives.
In reviewing these slides Chilmark was struck by the four models used to represent HIEs today (see below). First thing we thought of upon looking at these models is: These models only represent what is being built today and more importantly, completely ignore the consumer/citizen and their future control of personal health information (PHI)? Where is citizen’s PHR or personal health cloud account (Dossia, Google Health or HealthVault)? Are these PHRs or health clouds not HIEs in their own right, albeit truly citizen/patient-centric? The HIE Workgroup appears stuck in old models, models that have struggled to prove themselves relevant and viable to the market.
Roughly a week after this meeting, on July 22nd the eHealth Initiative (eHI) released the results of its annual survey of HIEs, the sixth year they have done so. Through the generous sponsorship of HIE vendor Axolotl, one can get the full report for free and on Aug 4th, eHI will host a free webcast to go over the results. While the report had many positive things to say about the current state of HIEs, claiming that more are operational, more are showing some form of return on investment (either soft or hard) and that more data is being exchanged, Chilmark found it interesting that the primary issue facing HIEs today is “Privacy and Confidentiality.” With stricter HIPAA consumer consent criteria forthcoming as the result of the passage of ARRA legislation, this will only become more difficult.
Another small bit of information tucked into the eHI report are some numbers regarding consumer access to their PHI within an HIE. Of those 67 operational HIEs today, a paltry 12% have some form of consumer access to their PHI. Might not greater engagement of consumers by these HIEs lend not only public support for HIEs, (and future funding as well as relevancy- both still a nagging issues) but also address the biggest issue HIEs are confronting today, privacy and confidentiality?
Then one goes back to look at the models presented by the HIE Workgroup, models that have no place for the citizen. These are not models that the public can readily support for the public has been completely left out of the equation. And ARRA legislation has given $300M in taxpayer/public money earmarked for HIE development over the next two years…
Hold on here, we need a major rethink on what an HIE is, who an HIE serves and the relevancy of HIEs to the public interest.
Granted, Chilmark will cut the Workgroup some slack as they are, we believe, making these recommendations with the best of intentions. What is troubling though is that this Workgroup has failed to create a vision for HIEs that not only supports MU criteria, but more importantly, supports the citizen’s need (and possible desire) to take greater stewardship of their health records. What the HIE Workgroup has proposed instead is a continuation of the status quo, which is truly unfortunate at a time when we as a nation are looking for new approaches to better engage citizens in self-managing their health, fostering healthy behaviors and empowering them to make wiser healthcare decisions for themselves and their loved ones.
It is time to move away from such paternalistic models so prevalent in healthcare today and represented in what the HIE Workgroup presented on July 16th. Let us create a new vision for HIEs that puts the citizen in the center. Thankfully, there are some thoughtleaders adopting this model, best represented by the efforts in Washington State, which now has three healthbanks, two using HealthVault the third using Google Health.

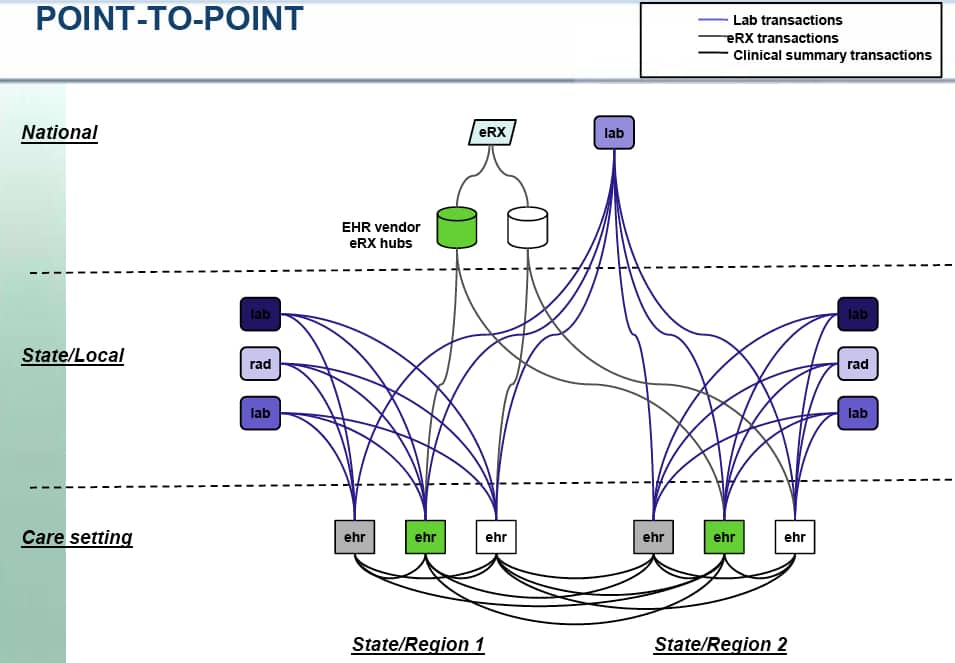
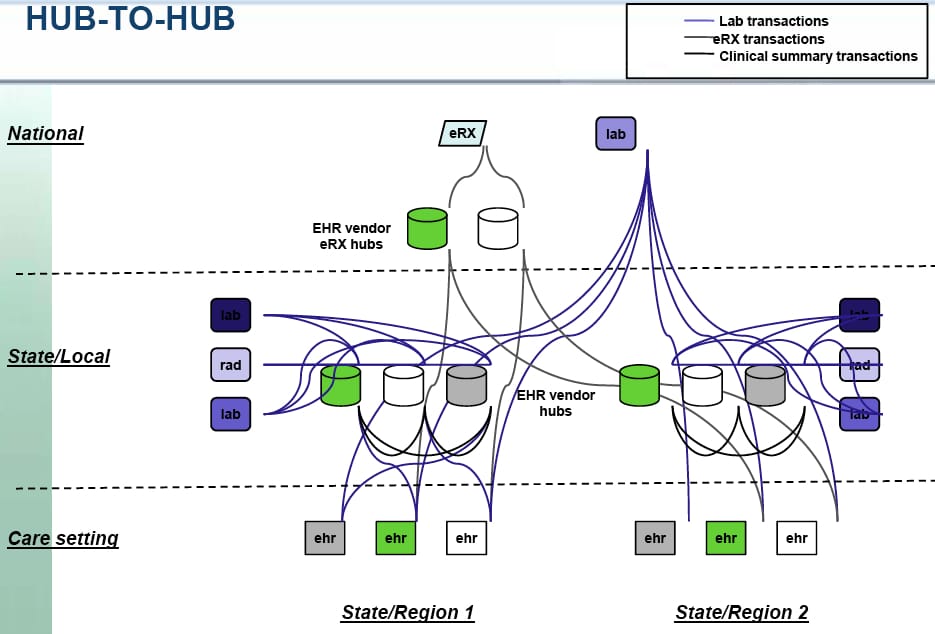
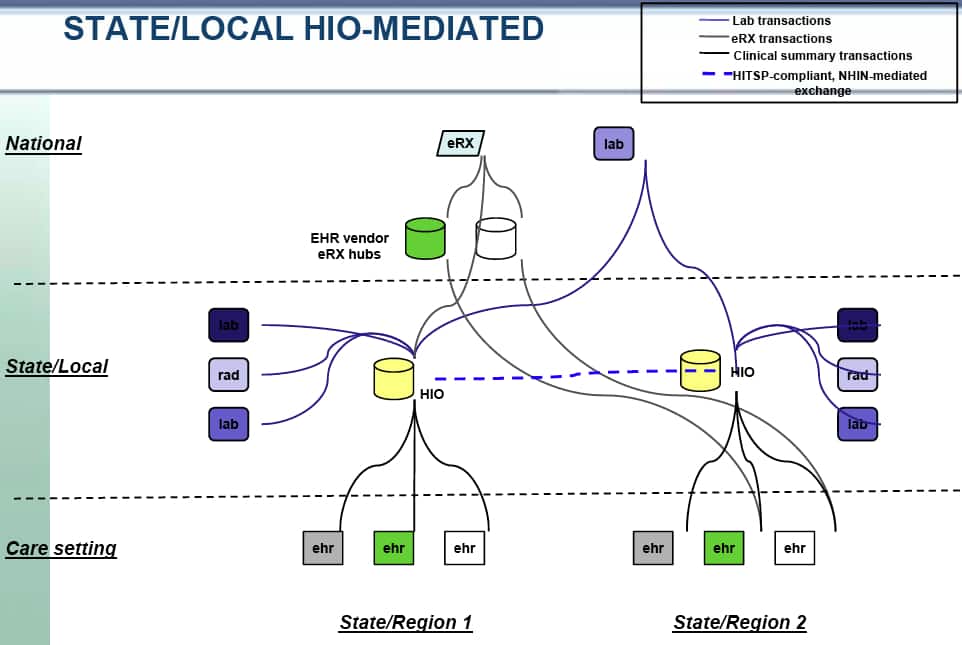
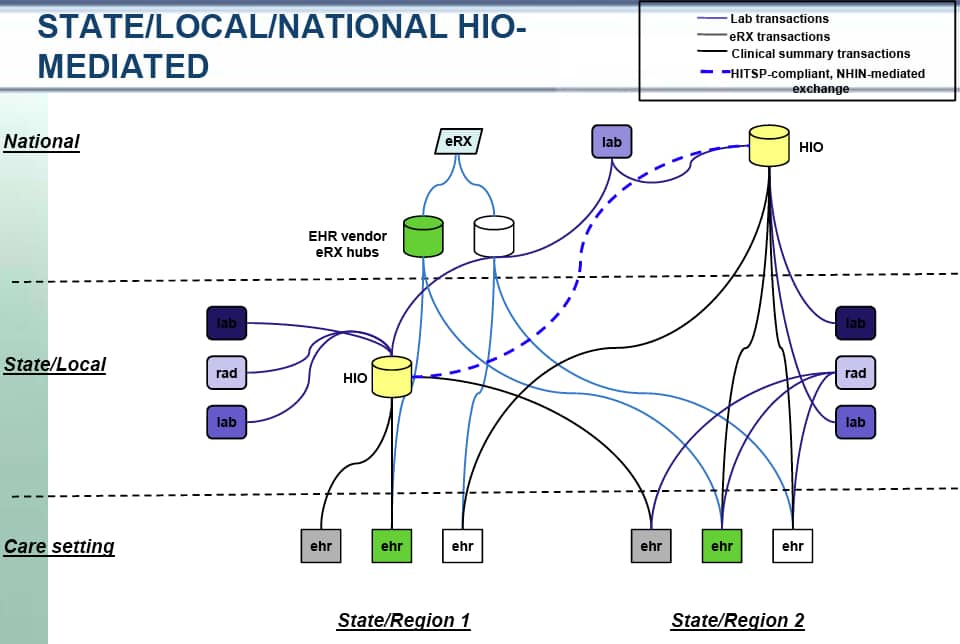



Nice HIE analysis. We have a leading RHIO in Rochester NY who’s hallmark is the cooperation of ALL stakeholders — hospitals, employers, insurers, doctors, Rx, labs, radiology, etc.
Follow the healthcare debate and the critical data about health care delivery at http://www.ilovebenefits.wordpress.com
Excellent analysis, and your graphics certainly describe the complexity we face in the “new world of electronic health records.” That said, these challenges will not be insurmountable if the right processes are in place to dissect and develop a road map to the desired state.
I recently posted a brief commentary with a 3 phase recommended path of action entitled “EHRS: A difficult task or a pipedream at http://www.myhealthtechblog.com/2009/07/ehrs-difficult-task-or-a-pipedream.html
The 3 phases recommended are: 1) Develop the “As-Is” picture that describes where you are today; 2) Develop the “To-Be” picture that describes where you want to be and where you are going (i.e. with EHR implementation); and 3) Develop the “Road-Map” which is described as an iterative process, accomplished in phases, and is revised as new information is learned or recognized.
Thanks for your excellent synopsis. Current models for health information exchanges are antiquated and flawed. As you so aptly point out, the patient/consumer has been entirely left out. Fortunately, the tide is beginning to change. As I pointed out recently on HealthBlog, a new model is emerging. See http://blogs.msdn.com/healthblog/archive/2008/07/22/a-possible-sea-change-in-thinking-on-how-to-share-health-data.aspx and also http://blogs.msdn.com/healthblog/archive/2008/07/22/a-possible-sea-change-in-thinking-on-how-to-share-health-data.aspx
Bill Crounse, MD
Obviosuly from our perspetive in WA State this is an excelent analysis however needs more “data points” that we hope we can contribute to as we learn more about health record banks (HRBs) and their potential utility as HIEs over the next six months or so. As a point of clarification, there are actually four HRBs in WA State. Three are funded through the state (grants) and the lion’s share of resources are coming from the communities,
Microsoft and Google (INHS, Spokane; Community CHOICE Wenatchee; and St Josephs, Bellingham). The fourth pilot is DoD Madigan Army Med Ctr in Tacoma, WA.
Thanks for a great blog post. I would like to add a couple of thoughts.
First, the hierarchical approach of the current HIE architectures mirrors the old phone system. The telcos built local exchanges (those windowless brick buildings) to which consumers were connected via copper. These local exchanges are the choke points that the intelligent distributed routing system called the Internet rendered unnecessary. Unfortunately the exchanges are still necessary….to protect local service monopolies.
Taking this analogy a bit further what we need is semantic health connectivity enabled through the cloud. This cloud based connectivity will enable the really valuable thing–care coordination. The cloud can “drizzle” content (images, HL7 messages) wherever it is required for analysis.
I would also like to amplify your point about the complexities of information sharing agreements in the context of the current HIE architecture. I suggest that you take a look at the space based architecture of the recently completed Tripcom project in Europe. This offers a much simpler, elegant, and dynamic model for sharing health information.