Key takeaways:
- Patient engagement has come a long way for those organizations looking to move beyond early models of the patient portal propped up by meaningful use – but it still has a long way to go.
- Patient relationship management is more than just CRM for healthcare, and vendors from numerous healthcare core competencies all approach PRM from different perspectives.
- Market fragmentation will limit widespread PRM adoption for the next 24 to 36 months – but adoption will be methodical and deliberate, not slow.
About 18 months ago, Chilmark Research published a report encouraging the healthcare industry to push patient engagement technology beyond the portal. Our report outlined how existing solutions were not ready to support the types of engagements (frequent, bidirectional, mobile, and increasingly virtual) outside the traditional healthcare setting that are necessary to provide coordinated, value-based care to patients with varying degrees of health status and technological expertise.
We predicted it would take until 2020 for solutions to support this level of engagement. By 2018, we expected to be entering an interim phase broadly defined by pilot programs, incremental improvements to functionality, and increased interest from regional healthcare organizations (HCOs) and other “smaller” players.
Well, 2018 is here, and our expectations have mostly been met, as we detail in our forthcoming report, Patient Relationship Management: Higher Stakes Than CRM (Update: Available now! The report can be downloaded by CAS subscribers or purchased a la carte). While adoption has been slower than anticipated, we have been surprised at the pace of improvement, which has been driven in large part by the emergence of vendors approaching engagement from different perspectives.
PRM adoption will remain incremental over the next 24 to 36 months. However, the pace of adoption will be methodical and deliberate, not slow.
Many factors, and many players
Due in large part to EHR implementation motivated by meaningful use, the portal has driven and enabled patient engagement efforts over the last decade. But the EHR’s original role – capturing data at the point of care to streamline billing – does not on its own lend itself to a better engagement experience, especially for engagements that do not constitute billable encounters. That’s a major reason only one in four patients access their health data electronically even though nearly 90% of HCOs offer them the ability to do so, according to Government Accountability Office data.
Numerous factors have motivated healthcare to rethink engagement in between care episodes, namely the following:
- Shift to value-based care models and risk-based contracts (from both public and private payers).
- Pressure to better manage (or even prevent) chronic conditions.
- Rapid consumer adoption of mobile technology for both personal and professional use.
- Increased patient responsibility for premiums, deductibles, copays, and other out-of-pocket costs.
- Importance of patient acquisition and retention, especially amid HCO merger and acquisition and in competitive markets.
With numerous motivations to rethink engagement, it shouldn’t be surprising that vendors with multiple core competencies have stepped up to help HCOs rethink engagement. All told, Chilmark Research identifies seven core competencies, all of which contribute to or have a place in a theoretical “stack” of functionality. Vendors traditionally focus on one of these seven sub-segments of engagement. (See Figure.)
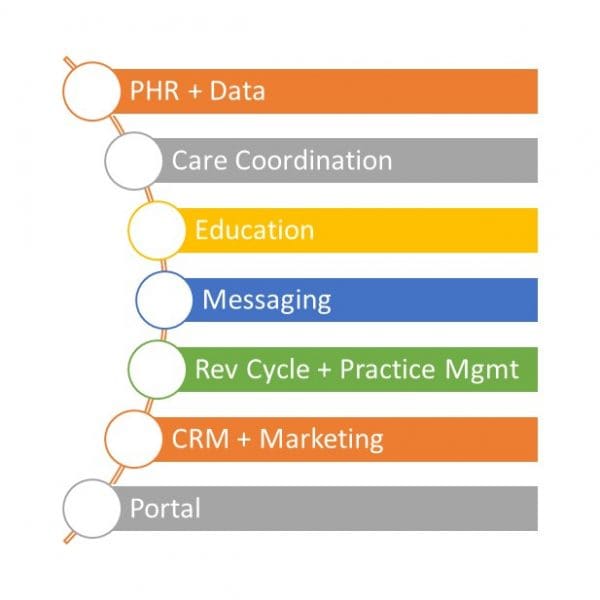
To provide a complete engagement solution, information should flow freely among the stacks. And information should be comprehensive: Care plans, in-network service eligibility, medication reminders, synced device data, care gaps / social determinants of health, intake forms, and specific condition management interventions – the list goes on.
As reflected in the title of our report, we refer to this collective stack as patient relationship management. The name is similar to customer relationship management, but true PRM is more than just “CRM for healthcare.”
Yes, PRM uses predictive modeling to identify patients to target with products or service offerings, as CRM does. Yes, PRM measures the downstream results of these targeted offerings and lets HCOs modify engagements accordingly, as CRM does.
However, CRM’s support of the “customer journey” is largely limited to the products, services, and people that a particular company (plus its closest partners) has to offer. To support the “patient journey,” PRM must extend beyond what an HCO traditionally offers. It must intersect with patients’ needs outside of the HCO setting, in between care episodes, as they live their everyday lives.
Filling the gaps
As noted, vendors’ efforts to support the patient journey typically focus on one of the seven sub-segments of engagement functionality. This has caused substantial fragmentation: Not only is there no dominant vendor across the sub-segments (out of at least several dozen PRM vendors in all), there is no dominant sub-segments of vendors as a whole.
This high degree of fragmentation is set to impact the PRM market over the next 24 to 36 months in three key ways.
One, PRM adoption will remain incremental. However, we would describe adoption as methodical and deliberate, not slow. HCOs will look for solutions that address clear patient engagement problems, whether it’s low scores on quality metrics, poor outcomes after elective surgeries, or large and disengaged prediabetic populations. HCOs will want vendor partners for pilot projects – but they will want mature partners for fully baked pilots. The process of throwing projects to the wall to see if they will stick will be left to internal innovation centers or early-stage startups working with affiliated incubators.
Two, PRM vendors will fill the gaps in their solution sets in order to demonstrate that maturity. Some vendors will opt for internal product development – such as EHR vendors continuing their pivots toward analytics, care management, and population health management. Most, however, will focus on partnership with leaders in other core competencies (particularly education, messaging, and personal health record management) as a way to fill these gaps.
Three, with both the appetite for IPOs and the prospects of unicorn-like growth softening, many single-function PRM vendors will face the choice to get acquired or go out of business. (To be fair, the same is true of point solution vendors across the entire digital health landscape.) This uncertainty may temper HCO enthusiasm to invest in an unproven vendor – or one that has succeeded enough to catch the eye of potential buyers.
Progress, but work to be done
These PRM market trends suggest that our prediction from the fall of 2016 holds true in the winter of 2018. We are still more than two years away from widespread adoption of comprehensive patient engagement solutions that can support coordinated, value-based care.
To do this, PRM solutions need to do two things:
- Meet patients where they are. The industry is getting there – and, admittedly, faster than we had anticipated 18 months ago. Bidirectional messaging and appointment scheduling, two of the biggest “asks” that patients have, are widely available in PRM solutions.
- Help patients manage their health and wellness on their own terms, outside the HCO setting. This has proven more difficult. PRM is making strides in these areas, by offering access to care plans and integrating medical and fitness devices, but support is neither widespread (not all vendors offer it) nor universal (not all vendors that offer it do it the same way). Plus, mere access to a care plan is not the same shared responsibility for a care plan – which is also not the same as self-sufficiency.
Progress has been made, but PRM vendors and HCOs still have work to do to meet patients’ needs. Our report provides many more thoughts on what it will take to make that happen. In the meantime, we welcome your thoughts.




0 Comments