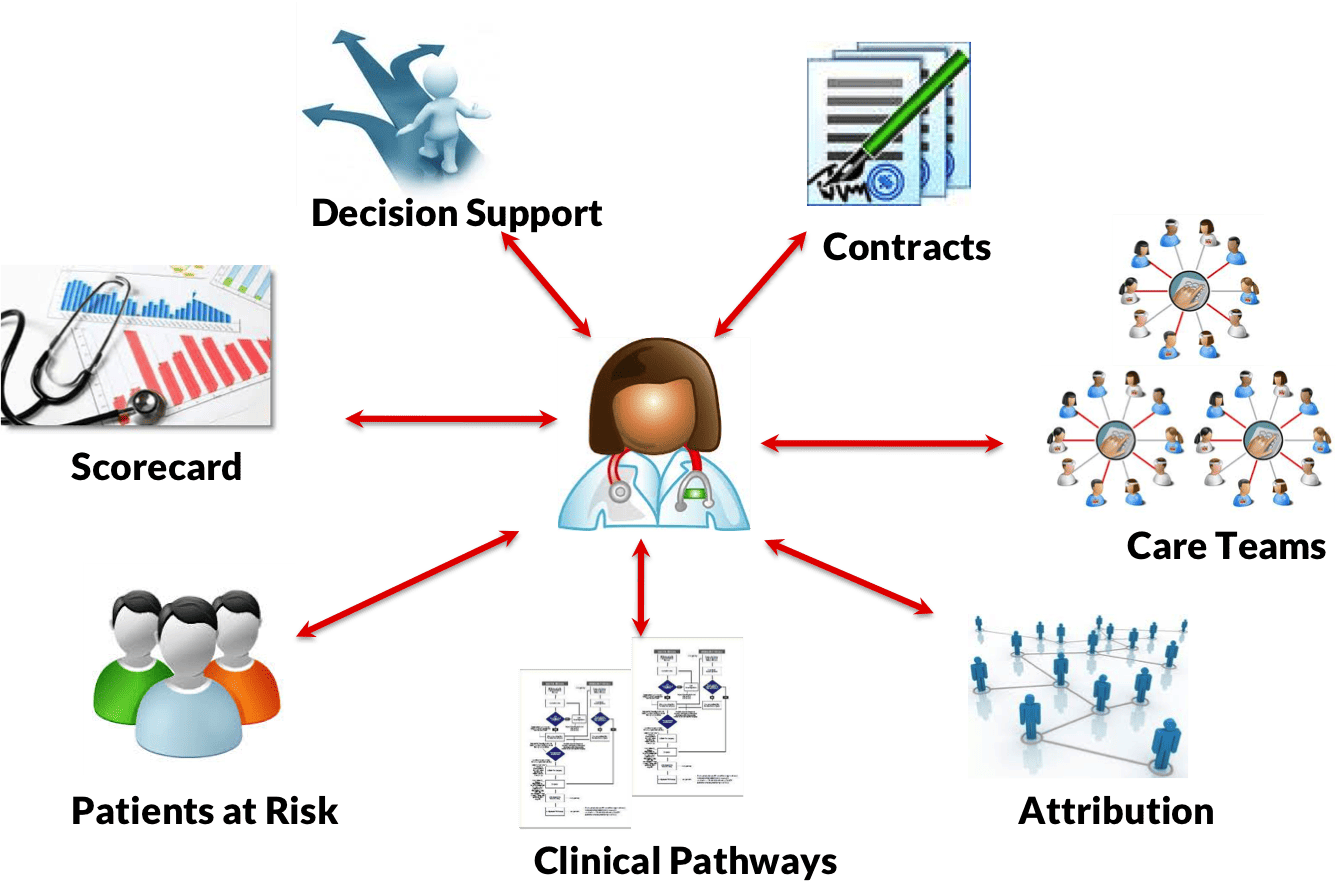
In this Chilcast episode, John Moore sits down with Deepak Sadagopan, COO of Population Health at Providence and CEO of the Providence Medicare ACO, Health Connect Partners, to discuss the strategic imperatives for healthcare executives navigating the transition to value-based care (VBC).
Allscripts — Stabilize, then Proceed with Innovation
At the recent Allscripts Client Experience (ACE, #ACEHHS18) conference, the company gave us a day...
Provider Directories: An Opportunity Fraught with Challenges
A primary goal of insurance expansion under the Affordable Care Act was to improve access to healthcare. Yet as thousands of people are finding, simply having insurance coverage does not guarantee that ‘the doctor will see them now.’
athenahealth Acquires RazorInsights: Can athenahealth Succeed Where Others Have Failed?
Success? On Wednesday, January 14, athenahealth announced it will acquire the cloud-based EHR...
Cerner Acquires Siemens: What can we Expect?
Chilmark Bight On August 5, Cerner announced its intent to acquire Siemens Health Services (HS)...
Use As Directed: Getting the Most Out of Patient Engagement Technology
Adoption Strategy Healthcare organizations (HCO) are slowly beginning to approach patient...
Free Research: Migration to Clinician Network Mgmt
Last summer we published another edition of our popular Health Information Exchange (HIE) Market...
Measuring Patient Engagement
Rise of Consumer Engagement As Healthcare organizations (HCOs) begin to go “beyond the portal”...
Analytics, Pop Health & Painful Feet at HIMSS14
HIMSS14…. brought me to the highest of highs and the lowest of lows. As in HIMSS past, I found...