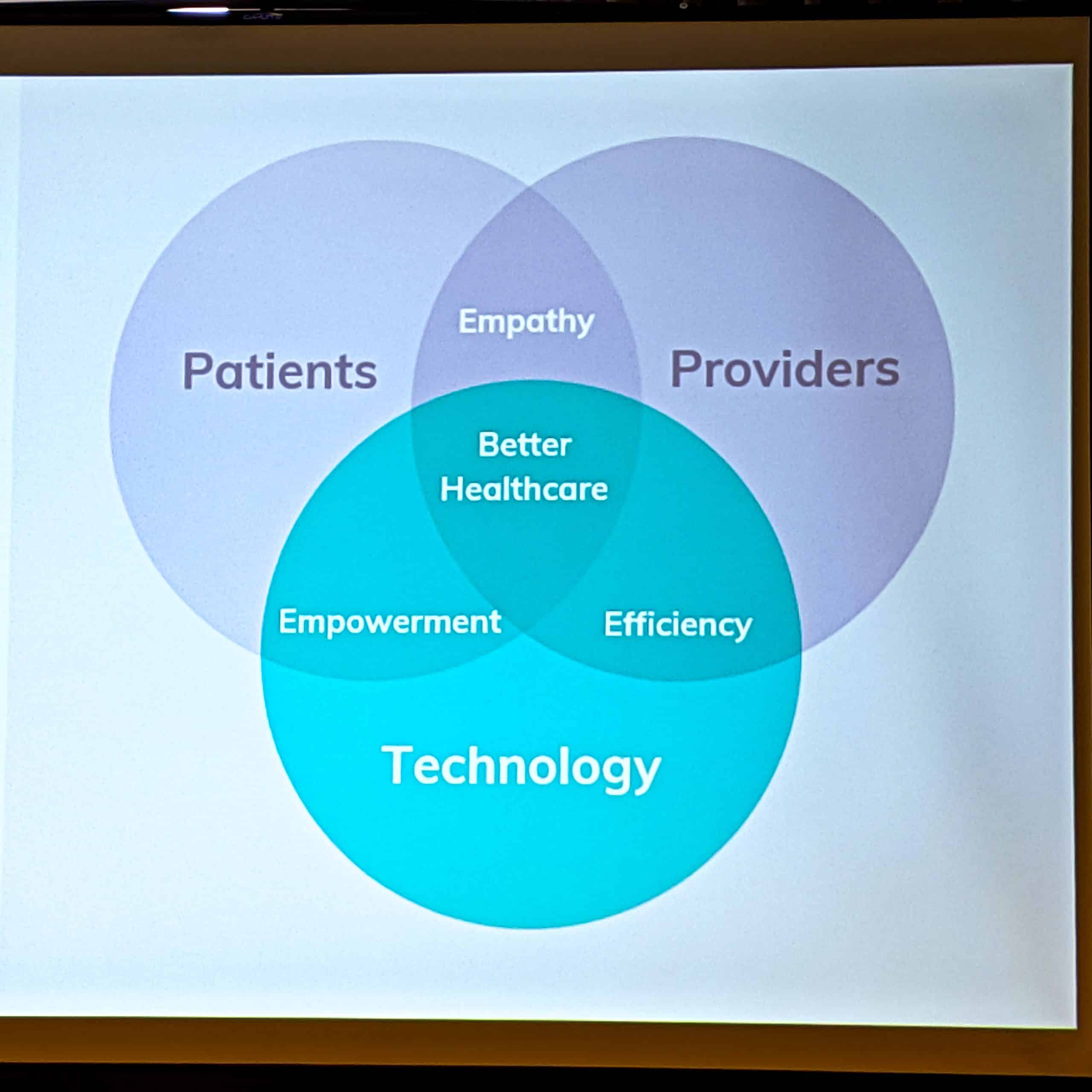
In this webinar, Chilmark's Research Director and lead report author Brian Murphy presented key...
Claims Analytics Will Soon Not Be Enough for Effective Performance Improvement Programs
The organizations responsible for paying for healthcare – health insurance carriers, health plans,...
Focusing on the Real World at Expo.Health
The second annual Expo.Health conference was held last week here in Boston. Its emphasis on...
Healthcare Provider Analytics and Reporting: Expanding Beyond VBC Use Cases
We will release our newest report, 2019 Healthcare Provider Analytics Market Trends Report, in the...
A New Take on Engagement: Aetna and Apple Launch Attain
On Tuesday I had the pleasure to be at Aetna - CVS Health’s grand announcement for Attain, an...
Chilmark’s HIMSS’19 Recommended Sessions
Once again, it is that time of the year for our annual pilgrimage to HIMSS. While many attendees...
What Are Bundled Payments and Are They Here to Stay?
Key Takeaways Current vendor solutions are limited and generally require additional advisory...
How will Proposed Changes to CMS Telehealth Reimbursement Affect Adoption?
On Friday, October 26, the Centers for Medicare and Medicaid Services (CMS) announced several rule changes that affect how telehealth services will be covered under Medicare Advantage (MA) and the Medicare prescription drug program (Part D). These changes are in direct response to the Bipartisan Budget Act of 2018, which eliminated historical restrictions on telehealth reimbursement, and are intended to “improve quality of care and provide more plan choices for MA and Part D enrollees.”
How to Succeed with a Provider-Sponsored Medicare Advantage Plan
[Guest Post] Health system and health plan leaders across the country are asking the same question: how will our organizations survive and thrive in a value-based world? As the shift to lower-cost settings accelerates and the population becomes older and sicker, organizations are seeking new ways to manage costs, generate income and control quality.