Conservative Predictions Result in More Hits than Misses
By: John Moore & the Chilmark Research Team
Looking back at our end-of-year predictions for 2021, I am not particularly enthused. Sure, we did a great job foretelling the future last December, with a batting average of ~ 0.620. But I have a problem with those predictions as the owner of Chilmark Research and director of our content. Frankly, we did not push ourselves to make predictions that were as edgy as I typically like to present to our loyal followers. Maybe it was COVID, maybe it was a holiday party hangover (oh right, no parties last December due to COVID). I know not the reason but am a bit disheartened by our lack of creativity. We will try quite a bit harder to push boundaries for our 2022 predictions coming later this month.
Now on to a review of our hits and misses.
*HIT* – COVID-19 hangover lasts far longer than expected.
As we enter the age of Omicron, COVID just keeps on going. We’re practically losing count of how many waves we have gone through to date – something like four… it’s beginning to look like COVID has no half-life and will be around for some time to come.
*HIT* – The unequal burden of disease for COVID-19 for minorities will intensify interest in SDoH and services that directly impact the disease burden.
Solid hit here, as healthcare organizations, payers, policy makers and IT vendors alike all look to address health disparities that COVID laid bare. We have a long ways to go in addressing SDoH in this country, but the Bipartisan Infrastructure Investment and Jobs Act makes some good progress.
*HIT* – Shift in focus of health systems from acute to ambulatory.
This is one of those lazy ones I mentioned previously, as this has been trending for going on two decades now. Recent CMS rules on site neutrality only add fuel to the fire.
*HIT* – Commercial payers and even Blues step up acquisition and partnership activity targeting the ambulatory sector.
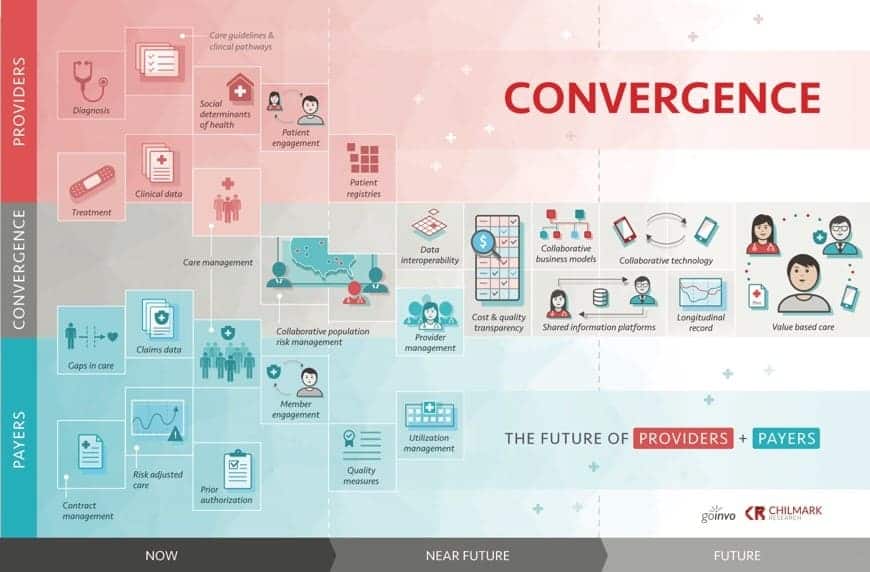
Well, this was another one of those exceedingly easy predictions to make, especially since we at Chilmark having been talking about convergence between providers and payers since 2017. I cover my head in shame at how obvious this was at the time of original publication.
*HIT* – Remote patient monitoring (RPM) remains a sideshow.
Despite the best intentions of many advocates and pundits for the future Internet of Things (IoT), of which RPM is a subset, the change management issues associated with effective deployment of such remain a significant challenge. Expect innovation on the edges, e.g., capitated Medicaid.
*MISS* – Self-insured employers will drive non-telehealth virtual care.
Employers did not step up to the plate in 2021 at the level we predicted, so they are out. That being said, we are seeing marked interest by the life science industries in electronic, patient reported outcomes (ePROs) to facilitate clinical trials and real-world evidence (RWE).
*MISS* – Maturation of the FDA’s thinking on software-as-a-medical device (SAMD) is creating a clearer path for AI vendors in the clinical decision support/remote patient monitoring space.
The pace of federal change can often stymie innovation. Clearer FDA guidance on SAMD and in particular, AI vendors, remains elusive. The latest set of guidelines is still thin on details. There are other paths to legitimacy – like self-policing. See forthcoming 2022 predictions.
*MISS* – Visages emerge of converging FinTech and HealthTech to optimize revenue.
What can we say? Healthcare is complicated. Despite efforts to improve patient workflow as it pertains to financing healthcare needs, we still have a long way to go. Pricing transparency and improving provider and payer interoperability are some promising signals, but the ideal remains wrapped in vaporware. There does appear to be a trend emerging that this will happen in 2022, so maybe we were just a little ahead of the curve.
*HIT* – 2021 will not be the year of the patient or member app.
This has almost become an annual swan song for the analysts here at Chilmark Research. Every year we hold out hope that we will be proven wrong on this count, but year in, year out, this prediction comes back like a recurring nightmare. At times, it seems like the only two things HCOs are interested in as it pertains to their patient app are billing and making sure a patient doesn’t skip their appointment. Follow the money…
*MISS* – CMS and its CMMI division will begin rationalizing VBCM.
Lots of talk coming out of CMS on the need to rationalize virtual based care models, but little has been acted upon. Maybe we are just a little early on this one, as the current administration has been preoccupied with infrastructure and “Build Back Better” legislative initiatives.
*HIT* – Digital health in the pharmaceutical sector will see more rapid adoption due to COVID-19.
Site-centric, clinical trials were de rigueur pre-COVID. That has all changed. Between the lockdowns and fear of contracting COVID at a clinic, life sciences companies quickly pivoted to virtual or distributed clinical trial models, with patients electronically reporting results from the comfort of their own homes. This model will continue to see rapid adoption with greater investments in new digital health tools to enable.
*MISS* – COVID-19 vaccine adherence problems drive the need for new analytics and care management.
Like many things, it is not always technology needs, which in this case were tertiary, when it comes to public health. Conspiracy theories, rumors, false claims, lack of concern, etc. are the leading cause of vaccine resistance. No amount of technology will overcome those issues. However, face-to-face conversations have proven most effective.

*HIT* – Virtual care consolidation continues.
Big fish (virtual care platform plays) continue to swallow smaller fish – niche virtual care vendors – especially in behavioral health. With continuing low interest rates and ready access to capital from VCs and PE firms, we expect this trend to continue into 2022.




0 Comments