Over the last few weeks there has been a lot of hype regarding mHealth. In late August Deloitte published an Issue Brief: The Mobile Personal Health Record (mPHR) that led to the conclusion that an mPHR will become the “killer app” healthcare app for the consumer. Then we have PWC who released their own report: Healthcare Unwired at the beginning of this week which stated that some 40% of consumers were willing to pay for wireless health solutions. Jane Sarasohn-Kahn did a nice write-up on the PWC report, though Paul McNamara may be closer to the truth on what consumers are really willing to pay for when it comes to mHealth-type solutions. And last, but cettainly not least is the plethora of mHealth conferences. As the fall conference season heats up, seems like one could go to some form of mHealth event every other week from now till Christmas.
As Eric Dishman of Intel points out in an excellent post, part of the problem may be one of definition, part of it al ack of truly trying to understand th market, its needs, the technology currently available to meet those needs and how does that technology become a part of the workflow of traditional care processes, or augment if not disrupt that workflow. Many questions that remain unanswered or poorly answered.
So is there really any justification for all this hype?
Yes and No.
Quite awhile back, when Chilmark first started looking into the mHealth market, we felt that indeed, there truly is something here and that provided the tools were simple enough, the value big enough that mHealth. It was at that time that we coined the term: Health is Mobile. Health does not happen when you are in-front of your laptop or desktop computer, it happens when you are on the move, going to an appointment, picking up a sick child from school, etc. Chilmark agrees with Deloitte that an mPHR like app has incredible potential, however, the lack of personal health information (PHI) in a common, computable digital format, (eg CCD or CCR) is a significant hurdle. There are also the issues of the need for a well-defined, simple to grasp value proposition for the consumer (see previous post) and subsequent business model(s) and a go to market/commercialization strategy that will make mHealth a sustainable success in the market. Not easy hurdles to overcome.
But there is significant change occurring and the rapid acceleration in adoption of smartphones is staggering. Recently, the market research firm IDC upped its 2010 smartphone growth projections from 44% growth to 55%. Then take a look at app sales on Apple’s iTunes. On September 1st Apple stated that 6.5B, yes, that’s BILLION, apps have been downloaded and 120M iOS devices (iTouch, iPhone, iPad) had been sold. This equates to 54apps/device. While many of these apps are for games and productivity tools, there are literally thousands of apps for medical, health and wellness purposes. What is particularly interesting about app download growth is that it is overtaking downloads of music. Maybe Apple needs to start calling iTunes iApps instead.
And then there is the story from Stanford Medical School where new med students this year have been issued an iPad in the hopes of replacing mounds of paper that are typically distributed to students for a course over a semester. The students seem to like it and even one of the doctors is quoted as saying towards the end of the article that the iPad is in an ideal form/function factor for a busy physician.
This may truly be key, for as the PWC report points out, most consumers would prefer to get their mHealth solution from their physician. Thus, if physicians get on-board in using something like the iPad, this could become a virtuous circle. First, the doctor will be able to easily create and update a patient’s record, digitally creating the content (PHI) that a consumer/patient could then use to populate their own mPHR. The physician’s familiarity and use of such technology will also drive a higher comfort level with using such in the process of care coordination and engagement with the consumer, including reviewing data in the consumer’s mPHR that may not have originated from their practice. Likewise, the consumer trusting in their physician and possibly with physician encouragement, will more readily adopt and use such a technology to better monitor and track their health or the health of a loved one.
Closing thoughts:
As Dishman points out in his post, too much is being put under the general rubric of mHealth. A clearer set of definitions are required to make sense of this market for today it is simply a mish-mash of terms extending from telehealth monitoring, which has been around for years, to novel apps on smartphones and the iPad to small, self-monitoring devices such as fitbit or even those devices that are embedded for say cardiovascular monitoring (defibrillator implants). Even PWC in its report, decided against the term mHealth, instead going with Healthcare Unwired to express a more encompassing view of the technology advances/capabilities arriving in the market.
But are we really doing anything breath-takingly new? On the technology front, not really, though the hype will have you think otherwise. Where the new really comes into play is in how will these mHealth/Health Unwired technologies affect the practice of medicine and the the delivery of care?This is where the real revolution will occur. This is where it gets interesting. So let’s not get so ga-ga over the technology, let us cool the hype-cycle and get down to the real business of understanding how these technologies will impact the delivery of care, the cost of care and the models of reimbursement, be it to the consumer, the physician, or the hospital. Now that is something to get hyped up about.
Giving Credit: Thanks to asymco for the great figure charting music vs app sales on iTunes.

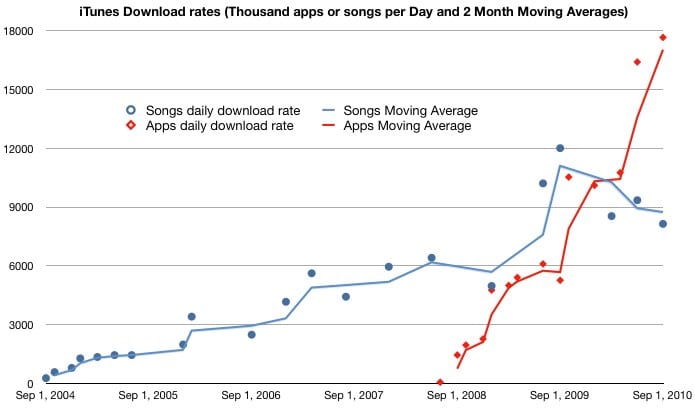



Wow! I am surprised to see the rate grow almost exponentially as oppossed to the rate that gradually increased when people download music. I got the iphone a few months ago and was impressed with all the apps Apple had to offer. I got a PHR for myself and it was free but the only thing the company offered was a card. I would rather go for a PHR that comes in flash drive and get automatic reminders, and I think that whether it’s an app or Medefile, or any other PHR company that it is beneficial to both patients and EHR’s. I hope to see a surplus in this field.
“So let’s not get so ga-ga over the technology”
Why not?
Look at the mess of our current healthcare system and how health services have failed to learn from other industries such as the banking, car hire, insurance or airline industries because of the vested interests of middlemen that are preventing patients from getting the health they deserve.
Mobile may be the newest and least understood mass media but it’s the change agent because it’s the first mass media that is personal, permanently carried, always on, has a built-in payment channel, is available at the point of creative impulse, is the most accurate at measuring its audience, can capture the social context of consumption and can offer augmented reality.
In case none of that’s getting you excited it’s also the fastest ever technology adoption in the history of mankind and it’s in the hands of patients and Doctors already…
Maybe we shouldn’t be looking a gift horse in the mouth?
Hi John, I agree that many of these technologies are interesting and have potential…may even be important and have the potential to improve the healthcare economy. But the problem remains that there is little reimbursement for the consumer side and I don’t care what survey is done, people don’t like to pay for their healthcare stuff. Reality shows us that this is typically the case. While consumers are being forced to pay more and more of their insurance costs, they have yet to demonstrate a willingness to pony up for serious healthcare apps or services on a sustained basis. Hell, people are even cutting out taking needed medications during the down economy. Until these products are integrated into the system as part of physician operating processes it is hard to imagine widespread uptake of those apps that require consumers to participate on a broad scale. Even the physicians have to be paid to adopt EMRs. I can’t imagine every hospital, much less IPA, in America is going to hand out free iPads, even if they should.
Smartphones will soon be the remote-control of our healthcare. These devices have more power than my first computer in college. We all talk about the “point of care” as being one of the most important issue with technology and healthcare. The phone in your pocket has the potential to provide both providers and patients “point of care” anywhere that they are and at any time. UCSD has a implantable Constant Glucose Monitoring device that is in FDA trial. The manufacture has stated that it will have the capability to transmit to Smartphones within a year.
I had the pleasure to participate on a panel with Eric Dishman of Intel several weeks ago. I spoke to him after the event about why Intel has not stepped up their effort in mobile Smartphones with Intel’s home health mobility efforts. He told be that Intel is waiting to see how the mobile health plays out. Several issues that he was referring to liability and FDA governance.
Mobile health as well as mobility is in it’s infancy, but changing quickly. Moore’s law time frame is being shorten. Culture is still the mediating factor in the exceptance and usage of these new technologies and service.
It is the business model that will ultimately drive this market. If mobile provides value it will become a norm in healthcare.
Jeff Brandt
http://www.comsi.com
One of the most important reasons for mHealth to become a driving force in out lives is the cost. Soon most people around the planet with have smartphones. Smartphones are powerful computers, my Android is a 1ghz machine capable of performing many task not even available in desktops in many Healthcare offices today. The next driving force is the proximity to the patient and provider. Humans take these thinks everywhere. Healthcare, reporting, collection, monitoring and advising anywhere anytime.
Smartphone will be the remote-control of our healthcare as well as our lives.
Jeff Brandt
The bottom line is that 99% of current mHealth apps have little to no value as all the data is siloed on the phone and the apps do not connect to a PHR, EHR or personal health platform such as HealthVault , Google Health or Dossia.
Connected apps have the potential to offer tremendous value in monitoring chronic conditions by providing real time clinician intervention without a brick and mortar patient visit.
Analyzing patterns of real time patient driven mHealth data will help providers monitor treatment regimens to identify effective and ineffective treatments and medications.
HealthSaaS is a pioneer in leading this change as we have created the first mobile chronic condition management app (Glucose Tracker +) that connects to our DiabetesPHR offering and Microsoft HealthVault.
Our patent pending Patient Outcomes Framework is the foundation for disease and condition specific Personal Health Records, white labeled offerings, telehealth support tools, and mobile applications. Connectivity to personal health platforms including Microsoft HealthVault and Dossia enable us to deliver solutions that improve results and lower costs for patients, employers, clinicians, provider networks and payors.
We are always open to discussing alliances with device and cloud based software vendors.
Frank Ille
CEO
HealthSaaS, Inc.
http://www.healthsaas.net
http://www.diabetesphr.com
John, Healthcare tends to oversimplify Technology with their terms. Take HIT, what does that mean? In most technical fields IT (Information Technology) equates the the person that is responsible for desktop maintenance, security and other support infrastructure. EHR is another, it was once just a data repository for patients records but now it could mean almost everything to patient provider communication to CDS. No wonder providers are confused. One stop shopping, is easy to buy, but can be hard to expand.
Regardless of what the killer app is today, one thing is for sure. Mobile changes everything. Healthcare is spending a lot of money on systems that will become obsolete before their installed. This is not HIT fault it is just the progress of Mobile. Mobile will lower the digital divide and reduce cost, but it will take a bit of time. My best advice is do your homework, look for systems that can adapt and are not silos, think ahead.
Jeff Brandt
http://mHealthBridge.com