This weekend, we will round the corner into America’s 239th birthday. Fresh off of two historic Supreme Court cases, many across the country are celebrating their newfound freedoms, from better access to healthcare (officially, this time…) to more equal treatment for our gay and lesbian citizens. Even as we celebrate these milestones as a nation, unfortunately there has also been ugly evidence in abundance over the last few weeks that we still have a ways to go before all the citizens of this great country – people of all ages, genders, ethnicities, and creeds – can enjoy true equality. That being said, we are a nation of progress; with our social, political, economic evolution comes more than a few growing pains.
In the social (media) corridors of health IT, there is a more focused rallying cry around a specific sort of “liberation.” The “Get My Health Data” initiative is a movement to improve Americans’ access to their own health care data. More detail is available on their website – but the story in a nutshell is that several high profile health IT leaders sparked a call to arms after a proposed amendement to the Stage 2 rules would have lowered the threshold for the ‘view, download, transmit’ requirement from five percent to just one single patient.
The movement was equal parts wakeup call and rallying cry: Despite the endless lip service being paid – by government offices, by software vendors, by large healthcare institutions, by industry associations like HIMSS and CHIME, and by many, many others – to improving everyone’s ability to simply and effectively “download their data,” unfortunately this issue has become more window dressing than actionable policy.
Over the years, the furor around “Blue Button” has really built itself up, with occasional updates from the VA and a handful of other institutions, or hollow “pledge” campaigns being used to prop up the vision. Groups like NATE are working on something, but each news brief I’ve read from them for the last year feels increasingly self-congratulatory and less and less “outcomes oriented.” If they were a startup they’ve have shuttered up by now. What is the “blue sky” vision, and where are the results against it? Forgive us for sounding ungrateful for their efforts – but frankly, all we care about *is* our damn data. In my experience (and countless others’) this has not come quickly enough.
Groups like CHIME and others continue to oppose holding providers’ feet to the fire – and to be fair, placing the entire burden of engagement on doctors’ behavior is probably a recipe for failure. Dr. Farzad Mostashari, has shifted his tone a little bit, saying that his vision for a “Data Independence Day” on this July 4th is not a one-day rally, but rather an ongoing, year-long effort to push people to try and get their data, collect and report the stories of what happens when they do so, and pool these stories into something greater – a meaningful vehicle to improve data access nationally (well, maybe “meaningful” is the wrong word).
Chilmark Research is optimistic that this is another move in the right direction, but skeptical of how much another “rah rah” campaign will do for the millions across the country who don’t pay attention (and rightfully so) to the latest microtrends in health IT patient empowerment circles. While we’ll support the cause, we would love to see a more dedicated, concerted, and specific effort by many of the wealthy and powerful organizations swimming around the healthcare ocean. Here are some specific thoughts as we go into the long weekend:

Key Bottleneck: Organizational Policy and Front Line Staff. A data liberation policy can be in place, but as many will attest, the folks who work at the front office have been around for decades in some instances. In many instances, their well-meaning “sorry we’re not allowed to do that”s are relics of an uglier, more paternalistic legacy of medicine. It is time for new education and training. How do we work the data access issue into the workflow of admins, nurses, and even physicians, so that they are on board to help educate patients on obtaining and using their PHI?
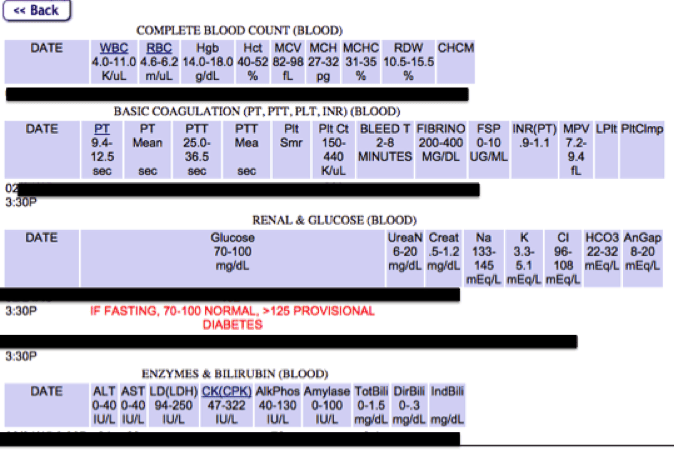
What my actual lab test results still look like in 2015. Ugly and Not Helpful.
Data Alone is Not Enough. Giving someone a .txt file of lab results is not a “base hit” – it’s a foul ball. It is meaningless, and worse, condescending. Without proper presentation, colorful and exciting visualizations, and some plain English explanations, this will be a waste of time. Patients need to understand swiftly and precisely what their data tells them. Otherwise we’re missing the entire point: We’re telling patients “here’s your data, we’re still the experts and without us you can’t do anything with this.” Health IT Vendors: this is all on you! Shipping a portal that doesn’t have automated visualizations to display data (built in, included at cost) is announcing (or underscoring) to the industry you don’t care about patients’ engagement in their health. Products speak louder than words. Please, do better. Can the #GetMyHealthData movement nudge this multi-billion dollar industry into action? Is it even willing to try?
Leadership: Who Will Take Charge? If data access is going to be systematized, an entity needs to take charge on corralling peoples’ past medical histories and putting them in one place for the patient to use. Will this/should this be the health plan, the employer, or the provider? Companies like Prime, Picnic, CareSync and others are working on this concept through technology and some elbow grease. Yet those solutions, even if they are successfully built, need to be codified into the broader system. The most effective way to ensure equal access is for one of the macro-stakeholders to simply own the task. We know this is much easier said than done. Again – this would be a nice area to see some high profile, multi-stakeholder collaboration.
What Are the Goals? Finally, as we launch into another tweet-filled frenzy for the next year, it will take more than a wishful petition and a myopic consumer campaign to push the envelope. Under national leadership from Farzad, Aneesh, and their other high-profile and influential friends, we’d love to see something more concrete:
- What changes need to be made to product design to allow better “flow” of data? How can we mandate or standardize them in every piece of certified health IT?
- What can we learn from Amazon, Uber, Google about building a set of data around an individual? How will these findings be applied to our PHI (and when)? Is it possible to truly, and safely “free the data” in a useable, publish/subscribe fashion that makes the experience seamless for the consumer?
- How do we operationalize use cases for patient data? How do we use it to get patients to set pre-visit goals, prepare questions for their caregivers, or share it with their pharmacist, or virtual doctor app, or weight loss coach, or whoever else might help them with their health?
Without a doubt, progress is being made. 10 years ago, patient-facing data was hardly even a concept worth debate. Today, while we are figuring out how to optimize data access, the broader goal is to leverage data for better health outcomes, better engagement, and more informed citizenry. As with all evolution, there are inevitable growing pains.
Happy Fourth of July, and happy #dataindependenceday.





Hi Naveen,
What your actual lab test results still look like in 2015 is not only “ugly and not useful”, it is exactly what they have looked like since medical computing began in Boston and Salt Lake City in the 1960s!
It seems obvious that proper test results presentation is essential for all physicians and patients seeking to optimize the value of the shared decision-making model of practice. The big problem is that EHRs (ambulatory and inpatient), PHRs (tethered and untethered) and HIE platform physician and patient portals are still using antiquated, time-wasting, infinitely variable reporting formats to display the cumulative results of diagnostic tests to both physicians and patients as incomplete, fragmented data that is hard to read and difficult to understand.
It’s not surprising that within the paternalistic medical practice model, the test result users have been powerless and the health IT system vendors have never had compelling financial or strategic incentives to correct this industry-wide, major clinical data management problem.
However, as the individual-centered, value-based reimbursement and provider-based financial risk era continues its nationwide deployment, private and public sector stakeholder collaboration to develop and deploy a practical solution, although not a trivial task, may finally become possible.
One logical solution that has already been prototyped is a clinically intuitive, standard reporting format designed to transform fragmented test results data into easy to read, complete, integrated and actionable information. With successful introduction of FHIR-based public APIs, competing ‘App Stores’ in a medical app ecosystem* and future releases of the FHIR Diagnostic Report resource that support cumulative results presentation, more advanced versions of a standard reporting format could include portable, reusable and shareable plain English test explanation apps for patients and workflow-integrated clinical decision support testing optimization apps for physicians.
* https://ehrintelligence.com/2015/03/09/is-creating-an-app-culture-the-key-to-ehr-interoperability/
Bob
Bob – sorry for the late reply, but thanks for your comment and your optimism.
I agree that the shift towards centralized, platform-driven data management will provide all stakeholders with a little more relief. What remains to be seen is whether that approach, too, falls victim to the myopic “competition” that doomed EHR interoperability. FHIR has been one of the great hopes of 2014-2015 – yet only time will tell if their use cases embrace the patient as an end user. To date, little evidence of that.
Naveen
I got access, download, messaging, and connected to nationwide HIE. Wisconsin rocks. Why? Because we all insisted on useable interoperability standards. IHE XDS and XCA based. Support Direct, but it is useless compared to a real network. Please investigate my claim. http://wishin.org