Convergence is a thesis that posits the successful path to risk-adjusted care requires realignment in provider-payer relations – that neither provider nor payer will truly be successful without the core competencies of the other.
Optimizing risk-adjusted care will require providers and payers to develop far deeper forms of collaboration to deliver not just insurance, or care but truly a higher, value-based health service in the markets they jointly serve. And within those markets lies the consumer/member/patient, the individual carrying an ever-increasing share of costs.
Disparate processes of providers and payers that are prevalent today do not readily lend themselves to providing a best-in-market, health service. Administrative burdens and duplicative processes abound. Lack of data transparency minimizes opportunities to personalize services and automate mundane tasks. It hinders care gap closures and often compromises critical population risk scoring.
One example: Payers, and increasingly providers, are each striving to minimize risk across their shared populations through more proactive care management. Each are proactively reaching out to at-risk patients/members to provide care guidance. But in doing so, they may unintentionally send mixed care messages and guidance to the patient/member leading that individual to question who is providing the best advice. This is far from an ideal consumer experience and at worse, may jeopardize their health.
Convergence is is not a new concept. Large healthcare providers such as Kaiser-Permanente (KP) have been vertically integrated for decades. Payers have likewise made a number of strategic provider purchases to build-out their own integrated services suite. Neither of these approaches has proven to scale nationally for a whole host of reasons. The “payvider model”, providers standing up their own health plans similar to KP, has been in vogue recently but may also be losing its luster.
What we are now seeing develop are deeper, strategic partnerships and joint ventures between providers and payers – partnerships that have seen a significant uptake in the last few years. Such partnerships are typically driven by local market-conditions. Anthem’s Vivity, a partnership with seven health systems in Southern California was motivated by the need for a service that was competitive with Kaiser-Permenente. Similarly, Geisinger’s recent partnership with Highmark is to counter UPMC’s expansion in the region.
What is the end point?
A core underpinning to any convergence strategy will be the exchange of data, data flow that is secure, automated, on-demand. Yet today, providers and payers have invested in separate technology stacks each having multiple data sources within. The IT infrastructure required to bridge the two disparate systems and associated data silos is nascent at best. Yet, it is unlikely that technology will be the key obstacle to data sharing and convergence. Trust and data governance will be. Overcoming those two critical obstacles will require strong executive support
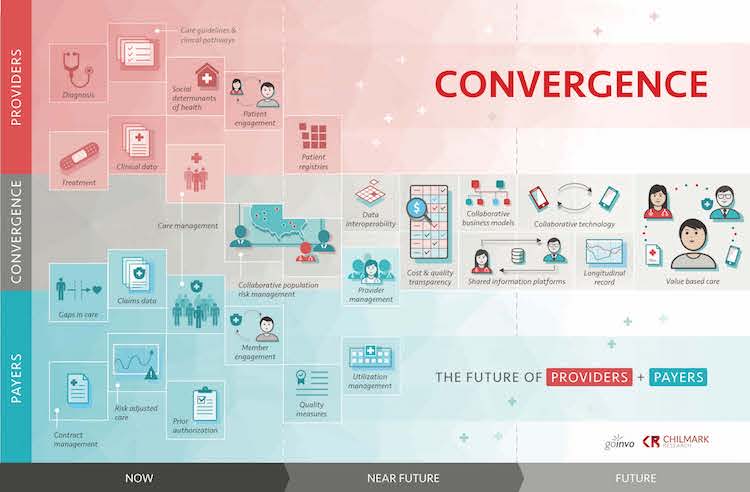
Working with the design firm Involution Studios we created the figure below to provide a visual perspective of where we are today on the path to Convergence and the ideal endpoint we envision for the future.
As the figure shows, a convergence strategy evolves from today’s current state of disparate systems and processes, to a model where providers and payers collaborate closely, sharing data to facilitate a myriad of processes that ultimately lead to accomplishing the quadruple aim of lowering cost, improving quality, improving access and improving the experience for key stakeholders, especially the patient/member.
The path to convergence will not be easy. There are few clear examples to draw upon; best practices are almost nonexistent for enabling a convergence strategy – experimentation reigns.
Our recommendations for those considering a convergence strategy (caveat, we may change our mind on some of these based on what we learn at our inaugural event – Convergence, being held next week) are:
- Have a comprehensive strategy with clear goals and objectives including top executive buy-in. The path to convergence will likely take several years and all participants must be prepared for some short-term pain for long-term gain.
- Do not boil the ocean. Target small, easy to accomplish early wins that deliver quick value. For example, prior authorization process, eligibility and referrals, rising risk with clear guidance to act at point of care, up to date provider directories are all major points of friction and opportunity.
- Ensure there is parity between provider and payer – if one has upper hand, strategy is likely doomed.
- Involve key stakeholders, especially those that are well-respected by peers, to allay fears of front-line providers who may be wary.
- Meet partners where they are, working together to achieve a common goal.





0 Comments