This report is now free to the public via the form below. To accompany the release of this report, co-author Jody Ranck hosted a webinar with end users on December 9, 2020.
Increasingly, providers and payers seek to address social determinants of health (SDoH) in their patient populations to lower utilization costs as value-based care becomes more prevalent. To do so, the providers and payers must engage with organizations capable of affecting changes in aspects of patients’ lives that traditionally existed outside of the scope of healthcare.
This report evaluates these solutions, identifying the strengths and weaknesses of options in the market and predicting how the market will develop in the future. Research in this report is based on interviews with executive leadership teams of solutions vendors, executives from the major EHR companies, and extensive secondary research.
Key Takeaways
- The steady march to value-based care (VBC) amplifies interest in solutions that contribute to utilization management strategies.
- Providers that wish to address patients’ social needs can do so efficiently through referrals to community partners. This is made dramatically easier with community resource engagement solutions.
- Integration with community partners remains the main barrier to implementation, given challenges with data governance. Legal and internal engagement issues also slow adoption.
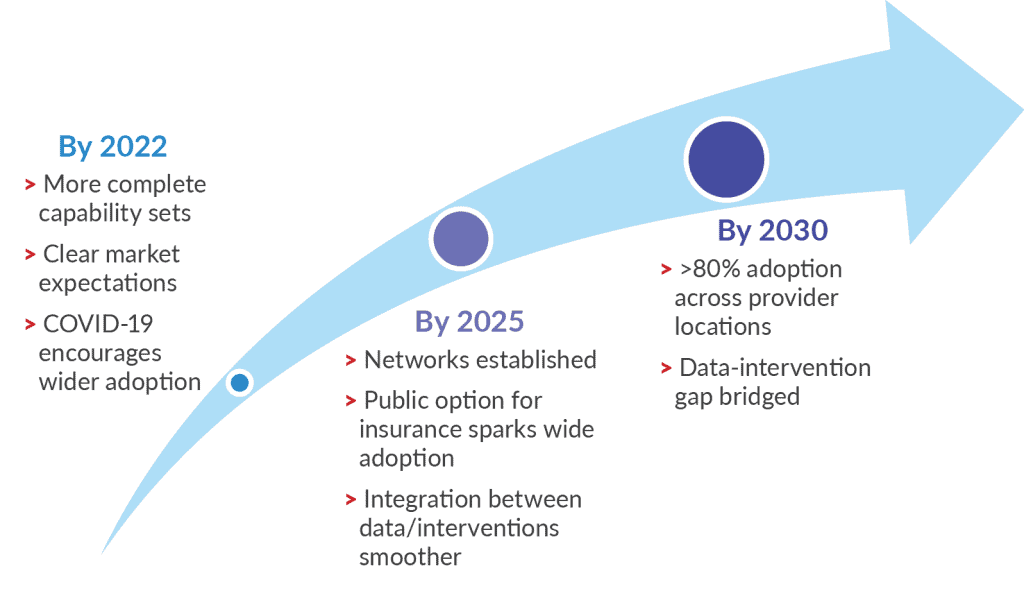
- The next two years will bring expansion of product capabilities with slow and steady growth in implementation as the market better defines standards for performance. Years three through 5 will see acclerated adoption and growth.
- Within five years, a public option for insurance will dramatically increase the rate of solutions adoption, culminating in >80% adoption in provider locations by 2030.
Vendors discussed: aunt bertha, Cerner, Epic, HealthEC, Healthify, NowPow, Signify Health, Solera, Unite US, Xealth
Download Report: