
After all, the rhetoric in the healthcare industry points directly at care coordination – loosely defined as the deliberate organization of appropriate, safe, and efficient care activities by a team that includes the patient – as the hallmark of value-based care. Focusing on care management, which centers primarily on evidence-based care plans, would seem like a step backward.
Well, it is. But it’s a necessary step backward. As we learned at HIMSS17, lots of people are talking about social determinants of health, but few are acting on them – and if they are, it’s for the purposes of risk stratification as opposed to more robust care plan development. More broadly, the community and social services so vital to providing coordinated care – the so-called next frontier of care management – remain far outside the view of all but the most forward-thinking healthcare organizations (HCOs).
It would be easy to cast blame at either HCOs or vendors (or both) for taking what appears to be the easy way out. However, as we learned, this step backward actually represents a necessary step forward for the care management market, and for healthcare delivery.
Simply put, the average HCO is nowhere near ready for longitudinal coordinated care. Reducing readmissions, keeping patients within their hospital network, hitting quality metrics, preparing for MACRA, hiring enough staff, optimizing the EHR – all take precedence. Fully embracing coordinated care is a low priority compared to proverbially keeping the lights on.
So vendors have adjusted their products in order to accommodate HCOs’ more pressing short-term needs. Tasks, interventions, and patient communications are increasingly tied to evidence-based care plans for conditions commonly associated with a hospital stay, not to more esoteric or longitudinal goals. What’s more, care management workflows remain largely analog – not because the technology doesn’t exist but, rather, because HCOs can’t yet be troubled to automate the parts of the process that might otherwise influence quality scores, chronic care management (CCM) reimbursements, or even where patients choose to seek care.
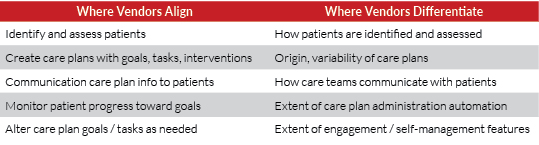
The end result has been a care management market that has aligned on HCOs’ basic needs but begun to differentiate in the ways that it addresses those needs (see Table below).
As the newly released 2017 Care Management Market Trends Report details, Chilmark Research thinks solutions that help HCOs address true coordinated care are still a few years away. Most HCOs remain cautious in a policy-making and business environment where little is certain. Expect vendors to work with their lighthouse customers to first develop and then roll out more robust care coordination functionality over time.
Sticking to episodic care management may seem like the easy way out, especially given how far HCOs have to come to provide more coordinated and value-based care, but it is in fact the smart approach for vendors today. Otherwise vendors would be pitching a solution to a problem that HCOs simply aren’t yet ready to address.
The report is available to subscribers of the Chilmark Advisory Service or may be purchased separately. For more information, visit the report sales page here.
In addition, Chilmark Research recorded a webinar summarizing the Care Management Market Trends Report on April 25. You can watch the recording of the webinar or download the slide deck.




0 Comments